This article shall discuss the numerous behaviors that the elderly engage in that places them at risk of falling. Some of the discussion will also focus on environmental factors that may contribute to a fall. Following this, various strategies and devices will be highlighted that can be utilized as part of a fall prevention program to minimize the risk of injury and death from a fall.
Not wearing prescribed glasses can lead to falls
Older adults suffer from a host of medical conditions that may impair their visual acuity, ability to differentiate between contrasting objects and stereoscopic vision. There are millions of senior citizens that wear glasses during the day to go about their lives and ensure that they are able to see all that is around them in their environment. However, when seniors and other adults go to bed, they take their glasses off as they prepare for sleep and place them on the night stand. The problem lies in that many people do not put them back on if they get up to go to the bathroom at night. On top of poor lighting conditions faced at this time of day, the addition of blurry vision and inability to differentiate between flooring and obstructive objects makes this a recipe for disaster. The question that needs to be asked is “if you wear glasses during the day, why do you chose not to at night when visual conditions are poor and it is even harder to see?” One’s glasses should be used each and every time when one gets out of bed, especially if these glasses are used during the day to minimize blurry vision or correct eyesight at various distances.
Poor visual conditions may cause trips over an unseen objects

Continuing on the topic of poor lighting conditions, it is important to evaluate the lighting setup in one’s home. It is common to find dark spots where light does not reach, even when all the nearby light bulbs are on. This is usually occurs on the middle of a staircase where there are no electrical sockets nearby and no landing to support a small lamp. In cases such as these, a small wall mounted battery powered motion activated nightlight (that was a mouthful!) can be extremely helpful in illuminating the way. More importantly, when one purchases a light bulb, one needs to see the amount of lumens a particular bulb gives off. What is a lumen you ask? Essentially it is a value that measures how much light is emitted by a bulb. The higher the lumen value, the brighter the room will be, while lower lumen bulbs may make a room seem dark even with multiple lights flicked on. Finally, it should be noted that most homes have poor lighting coverage because people expect one light source to be able to fill the entire room. This is not the case and darkened areas usually need to be corrected by adding more nightstand lamps and floor lamps.
Poor footwear can lead to trips and falls
Inappropriate shoes and footwear is another cause for concern with regards to falls prevention. Most elderly individuals have an obsession with slippers because they are easy to slip on and off. However, this means that they can come off easily even when one does not intend to remove them. Imagine trying to climb the stairs (an absolute no no whenever wearing slippers), or even just walking about throughout your home. In these two cases, one of three things can happen if you feel the slipper coming off your foot:
- You manage to put it back on without any problems
- The slipper comes off and falls out of the way, and does not interfere with your walking or use of stairs
- The slipper comes off and you step on the edge to lose your balance or it causes you to trip and fall
In the above examples, it is the last scenario that is the most dangerous. Because each fall has the potential to be deadly, especially for seniors that have a harder time recovering from injuries, action must be taken to minimize risks. A more appropriate alternative would be the use of a shoe with a built up heel that prevents the shoe from easily coming off. One must also take special care to ensure that the shoe is secured to one’s foot and that the laces are done. If laces are found undone, they need to be tied immediately before any further walking happens.
Poor pathway clearance can act as a barrier to safe mobility
A significant contributor to falls is an unclear walking pathway. While this is usually a concern in tight living quarters, it can also be an issue in larger spaces that are poorly planned. For instance, furniture can be arranged in such a fashion where it would act as a barrier to using a wheelchair or walker within the home. If there is not enough room to ambulate from one spot to another with the walker, one may abandon the device and attempt to use the furniture, walls and nearby objects for mobility support as they try to get to the bathroom or couch. This places seniors and those with mobility impairments at risk of falls.
It is best to arrange furniture so that spaces are clear and there are no obstructions in the way. This allows mobility aids to be used throughout the home and minimizes the risk of injury. Another common problem encountered with walker usage is that they are wide and may not fit through the bathroom doorways to access the toilet, bath or shower. This is sometimes the result of living in an older home which was not designed to accommodate such devices. Generally speaking the older homes tend to have narrow bathroom doorways (sometimes can be as narrow as 26 inches or less). These openings cannot allow a walker, whose width is usually anywhere from 28 to 31 inches, to pass through. As a result, walkers are left in the hallway while the user walks to the toilet or bathtub without any base of support. One easy way to resolve this is by using a pair of offset expandable hinges which allows the door to swing completely away from the vertical portion of the door frame where the door is secured. This adds two inches of more usable width to the existing doorway. In contrast, normal hinges prevent the door from swinging out of the way and reduces an already narrow doorway even further. With the added couple of inches, one may be able to enter the bathroom with their walker or wheelchair while maintaining safe mobility and balance.

Lack of mobility aid or inappropriate use can contribute to a loss of balance
As our bodies age, our ability to maintain balance and equilibrium tends to decrease for a variety of reasons. When this occurs, a mobility device may be required to support independent ambulation. However, making the change from using no mobility aid to using one is a difficult task and many seniors are resistant to the idea. The following are some examples that may interfere with the adoption of new gait aids:
- Many people overestimate their aging body’s capabilities and feel they do not need any mobility aids.
- Seniors feel a stigma is attached to use of canes or walkers. They see these tools as things used only by old people and do not wish to be categorized within that group.
- There is a lack of knowledge surrounding one’s physical needs and mobility aids
Ideally, a mobility assessment by a medical practitioner, physiotherapist or occupational therapist needs to be conducted to determine one’s level of mobility needs. From there, the equipment can be trialed with its user. During this process, training is an integral part of maintaining one’s safety. Because the mobility device is new to the individual, they may not have a grasp of all the necessary steps they need to take to ensure they are keeping themselves safe. For example, a common mistake made by new wheeled walker users is that they abandoning the walker instead of using it to get close to a sitting surface. Another mistake they made is that they forget to engage the brakes prior to leaving or using the walker. These actions place the user at high risk of falling and that is the opposite goal of using a mobility device. For this reason, it is important to receive training and have ample time to implement the recommendations into practice to ensure that the gait aid is being used correctly. That said, our memory starts to slip a little as we age and more education spaced out over several sessions can be used to maximize the knowledge retention and incorporation of safe mobility practices.
When selecting a mobility aid, it is important to consider the context in which it will be used. Some homes have narrow pathways and hallways, which may not accommodate wider walkers or wheelchairs. Another feature that one needs to consider when purchasing a walker is that some of them have the ability to fold slightly sideways whereas others cannot. This can slightly decrease their footprint as they are used to pass through narrow doorways and minimize abandonment normally seen with inappropriate devices. Lastly, during the trial, an assessment needs to be done to see if the mobility aid is able to meet the needs of its user. Sometimes a cane is not enough support and one needs to be advanced to a rollator walker.

In other cases, even a walker is not enough when the person should really be using a wheelchair. For this reason, it is important that the assessor is trained in measuring the person for mobility devices and able to provide the necessary safety training.
Polypharmacy can be a falls risk factor
With age comes numerous health conditions and deficits that sometimes our bodies need some assistance with. More often than not, this is in the form of prescribed medication and when complex medical conditions are present, one will be taking numerous pills at the same time. This is especially true when there are multiple co-morbidities. While even one drug may increase one’s risk of falling if it has a side effect of increased drowsiness or dizziness, imagine what multiple medications will do. Now consider that most medications tend to interact with one another and you have a recipe for falls. While pharmacists and physicians carefully screen for drug interactions to minimize any possible side effects, sometimes two meds that are contraindicated slip by. Sometimes aversive side effects may even occur after an extended period of being on a particular treatment regime. This is as a result of changes in how our bodies react to the medication after a long term exposure to its active components.
Whatever the case may be, it is important to always follow up with one’s doctor regarding any side effects one is experiencing, no matter how small. With medicine, it is always better to be proactive instead of reacting after a fall has occurred and the injury already sustained. For seniors that have difficulty leaving their homes, there are many community agencies that could provide a rapid response nurse to aid with care plans, which may include a comprehensive medication reconciliation plan. These nurses usually ensure that medications are cataloged correctly based on their name, dosage, frequency and route. This may include a careful review of discharge orders from hospital based doctors and the regular treatment plans initiated by a family physician. The goal of this is to ensure that people have an understanding of their symptoms and signs of illness within the context of side effects that may be experienced with medication use.
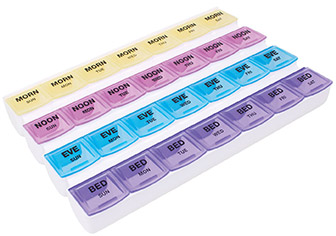
While the nurses have expertise in the field of medication administration and general med organization, pharmacists can also come into one’s home to perform a medication check and ensure that there are no additional concerns. When one is on numerous medications (usually 4 or more as per most healthcare guidelines), this tends to place people at higher risk of falling. A medication plan needs to be confirmed with all of one’s doctors and medication should never be discontinued without their instructions. Moreover, if there are multiple medications to be taken throughout the day, it can be increasingly confusing and difficult to keep track of whether a certain drug has been taken and what has not. For this reason some patients opt to have their medication placed into a blister pack by the pharmacy. These packs are organized into small bubbles that can popped open to take medication as prescribed. They are sorted by day of the week and time (typically breakfast, lunch, dinner and before sleep). This allows not only the patient, but also caregivers to monitor and ensure medications are taken as prescribed without missing doses by inspecting the bubbles that have been popped open. It may cost extra to fill the medication into a blister pack by the pharmacy, so some family members opt to organize the medication themselves on a weekly basis into a small pill organizer. It serves the same purpose as a blister pack, however the organizer is refillable whereas blister packs are not. Another drawback of the blister pack is that one needs to follow up with the pharmacy every week or two to obtain a new set of medications.
Strategies to reduce the risk of falling and minimize fall injuries
There are numerous aids and strategies that can be used to minimize injury if someone has a fall. Most importantly, one needs to be able to seek help rapidly. However, it is not uncommon for patients to have falls and lie on the floor for hours and sometimes even days before they are discovered by families or care providers. In these situations, people are unable to ask for assistance because they have no personal medical alert system or were not wearing the device at the time. Sometimes the alert pendant or wrist button is worn, but their arm or the device itself is thrown behind one’s back during the fall leaving the user unable to push the button to request for help. There are some services out there that have been trialing a feature where the system itself detects when a fall has occurred and calls for help automatically. That said, these systems are generally prohibitively expensive and are not guaranteed to work as designed (the engineering is just not there yet from what we’ve seen in the field). What usually works best is regular check ins either from family or neighbors.

In order for a check in to be valuable, it is important to place a lock box on the exterior of the home with the house key inside. The individual may be unable to open the door if they are unconscious or cannot reach the door related to an injury from the fall. In this case having the lock box combination relayed to first responders speeds up response time and care provision for the person. In situations where a lock box is not present, the ambulance crew will not have the equipment to break the door down to gain entry into the home. The paramedics must wait for the fire department to arrive on the scene to remove the barrier before the person can receive treatment. That said, with traumatic injuries, time is of the essence to successful recovery and patient outcomes.
Another useful tool in minimizing injury from a fall can be a padded hip protector. This is a special kind of undergarment that is worn at all times by those that are at high risk of falls. It is basically foam padding located at both hips whose purpose is to prevent hip fractures. While it may decrease the chance of injury, it is by no means a foolproof strategy and injuries can still be sustained.

Similarly if someone is at risk of falling out of bed, a fall mat can be placed on the floor to help cushion any falls. That said, the falls mat sinks in a little bit when walking on it, and that in itself can contribute to falls as it can affect one’s balance if walking on it. For this reason, it is meant to only absorb an impact and should be relocated when it is not in use. Times when the mat should be moved out of the way include during the day or when the person is getting out of bed with the assistance of a provider.

Of all the strategies and aids discussed, the most important falls prevention strategy is a careful assessment of one’s gait and balance. While it is ideal that an in home safety assessment be completed to assess mobility within the context of one’s environment, an outpatient or clinic visit may also be helpful in determining one’s mobility needs.
If one is using walls, furniture and other nearby objects for support while walking, then it may be time to consider a using a mobility aid. If one is already using a specific gait aid, then it may not be providing enough support and a different device may be needed. Whatever the case, an occupational therapist, physiotherapist or general practitioner would be able to offer some insight into one’s mobility needs. If well supported with an appropriate mobility device, one’s risk of falls will decrease, especially if the device is utilized in the correct manner as it was prescribed.
